Your Nursing Home Abuse and Neglect Lawyers
Your Christian Law Firm, Dean Burnetti Law represents Nursing Home Abuse and Nursing Home Neglect Victims in Polk County, including: Lakeland, Auburndale, Bartow, Haines City, Lake Wales, Mulberry, Polk City, and Winter Haven; in Hillsborough County, including: Brandon, Tampa, and Plant City; in Pinellas County, including Clearwater, St. Pete, Gulfport, Treasure Island, Largo, Oldsmar; and all of the surrounding Greater Central Florida and West Central Florida Areas.
Psalm 73:26 - “My flesh and my heart may fail, but God is the strength of my heart and my portion forever.”
A “nursing home injury” refers to either the abuse to and/or the neglect of the resident of a nursing home, assisted living facility, convalescent home, elder residential facility, senior living facility, retirement home, old soldier’s home, old age home, rest home, etc.

With the number of elderly living in Florida, people often wonder: What do I need to look for in a good nursing facility? Unfortunately, this question is an afterthought and arises only after an incident has occurred.
Remember, whether it’s one or both of your parents, or even your spouse, it’s critical for you (and other family members) to stay actively involved and vigilant to ensure your loved one receives the best possible care while in their nursing facility.
Before you sign any application, contracts, or documents to admit your loved one into the care of a nursing home, you need to tour the facility. There are federal regulations (overseen by the Centers for Medicare and Medicaid Services) in place which require skilled nursing facilities to provide the following to all residents:
- A clean, comfortable mattress;
- A bed of appropriate size and height;
- Bedding, which is appropriate to the weather/climate; A room with a window to the outside for natural light and orientation to the time of day, weather, and season; and
- Furniture appropriate to the resident’s needs, including a separate closet or clothing storage spaces.
These regulations also require nursing facilities to provide a “safe, clean, comfortable and homelike environment.” In other words, the goal is for these facilities to feel less institutional and more home-like, so residents can bring items and personal effects with them to help create a meaningful and personalized living space.
Beyond the above, you will want to utilize many of your senses on your tour of the facility.
What smells do you notice as you walk in the door or as you walk down the corridors past the residents’ rooms or through common areas?
 Unfortunately, nursing homes often harbor some not-so-pleasant smells. Many times, these are unavoidable, such as certain medications or diets making residents gassier than normal, in addition to the aging process which causes the elderly to be more likely to lose control of their bladder or bowels. However, if the facility reeks of stale urine, there’s a strong likelihood that it isn’t being cleaned properly or that the residents who wear incontinence garments are not being changed as often as they should be. Even worse, if many residents have bedsores, the nauseating smell of infection may be noticeable.
Unfortunately, nursing homes often harbor some not-so-pleasant smells. Many times, these are unavoidable, such as certain medications or diets making residents gassier than normal, in addition to the aging process which causes the elderly to be more likely to lose control of their bladder or bowels. However, if the facility reeks of stale urine, there’s a strong likelihood that it isn’t being cleaned properly or that the residents who wear incontinence garments are not being changed as often as they should be. Even worse, if many residents have bedsores, the nauseating smell of infection may be noticeable.
From the moment you enter the facility, stop and listen.
Take a moment, and really absorb the sounds you hear. Though residents moaning or yelling for help might be unsettling, that’s not necessarily a sign of mistreatment. However, keeping your ears tuned to how staff members address the residents may indicate something noteworthy. Remember, the generation going into nursing care these days came from a time when they were addressed as Mr. Johnson or Mrs. Williams. So, if the nursing staff calls them Sweetie, Honey, or Mama, the resident may lose dignity, may feel as if they are being “spoken down to,” and if dementia has started to set in, the resident may not even be responsive to the nickname.
Does the food look and taste palatable?
 While a meal might meet one’s dietary requirements, if it doesn’t taste good to someone who may be losing some of their sensory sensitivity (taste), or if it isn’t visually appealing to someone who may be losing interest in eating, that’s a definite red flag. While you’re touring the facility during mealtime, take note of how many residents are gathered in a common dining room, or if they are kept in their beds to eat. No one likes staring at the same four walls all day. Notice whether the residents are feeding themselves. If they are unable, is a staff member helping them eat? Sometimes, understaffed facilities don’t have the manpower to help feed elderly patients who are unable to feed themselves which often causes the patient to lose a significant amount of weight in a short time.
While a meal might meet one’s dietary requirements, if it doesn’t taste good to someone who may be losing some of their sensory sensitivity (taste), or if it isn’t visually appealing to someone who may be losing interest in eating, that’s a definite red flag. While you’re touring the facility during mealtime, take note of how many residents are gathered in a common dining room, or if they are kept in their beds to eat. No one likes staring at the same four walls all day. Notice whether the residents are feeding themselves. If they are unable, is a staff member helping them eat? Sometimes, understaffed facilities don’t have the manpower to help feed elderly patients who are unable to feed themselves which often causes the patient to lose a significant amount of weight in a short time.
How do the residents spend their waking hours?
As you tour the facility during the daytime, you want to take note of how many residents are still in bed. If there is a crowd of residents circling the nurses’ station or watching people come and go through the front door, that’s still better than them being stuck in their room all alone with a TV to babysit them. However, a quality facility will have a daily activity calendar for their residents. Activities can include such things as a live music and sing-along hour in a common room, BINGO, jigsaw puzzle time, a common TV and board game room for use during unstructured times, church and worship times, a Bible study hour, visits from local youth groups, visits from various animal handlers, an exercise hour, an outdoor time, a gardening hour, a walking tour, etc. Some facilities even have a bus that transports the residents (and their caregivers) to stores or concerts once a week so they can get out.
You’ll also want to pay attention to how the staff interacts with each other.
If the staff are rude to each other, they won’t think twice about being bad-mannered with a resident. Additionally, if the radio or TV playing in the background are not tuned in for residents but are rather playing shows or music for a twenty-something crowd, then you know those are really on for the staff and not the residents. Likewise, if a resident’s TV is tuned to a young children’s show, the staff is turning that program on, and in the process, are causing the resident to lose dignity by not allowing them to watch something they might have enjoyed when they still lived at home which was meant for adults. Finally, pay attention to how the nursing staff spends its time once all the charting and direct care has been finished for their unit. If you see a bunch of nurse’s aides grouped together giggling over something while the residents are stationed in wheelchairs looking bored, then that’s a problem.
Do you notice any bruising?
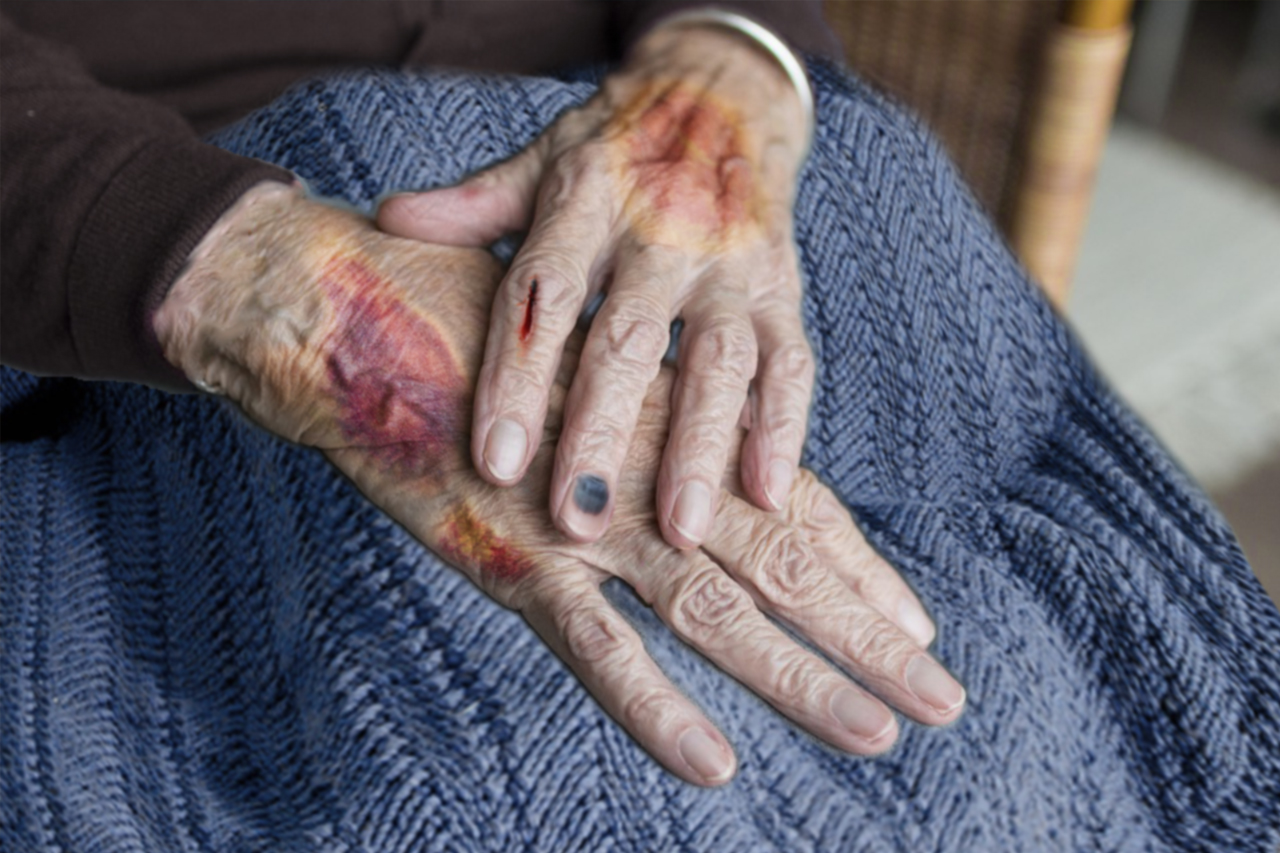 Every black-and-blue mark you see is not necessarily a sign of abuse. As people age, their skin becomes thinner and more fragile, and certain medications make them more likely to bruise easily. However, some contusions should not be ignored. Look for a hand or fingertip shaped bruises around the wrists or upper arms. Also, any handprint-shaped marks on any body part are unlikely to be caused by a fall and should be questioned.
Every black-and-blue mark you see is not necessarily a sign of abuse. As people age, their skin becomes thinner and more fragile, and certain medications make them more likely to bruise easily. However, some contusions should not be ignored. Look for a hand or fingertip shaped bruises around the wrists or upper arms. Also, any handprint-shaped marks on any body part are unlikely to be caused by a fall and should be questioned.
How does the facility handle a resident’s fall?
When you’re dealing with the elderly, falls can happen under even the best of circumstances, but it’s important to know how the staff reacts. Do they check for injuries? Do they help the resident get up off the floor safely? Is the resident checked later in the shift for injuries that aren’t apparent at first?
Is the staff overworked?
Don’t be afraid to come right out and ask the nursing assistants and other staff if they work a lot of overtime or double shifts. If so, there’s a red flag that the facility may be short-staffed which can affect the quality of patient care. Likewise, you can ask the facility director what their staff to patient ratio is, then compare it on the Nursing Home Compare tool at Medicare.gov. Lack of stuffiest staff can increase the likelihood that the staff is overworked and overly stressed.
Do you notice bedsores?
Sometimes, bedsores are unavoidable, especially as a resident becomes sicker and more immobile. However, if the resident is capable of being up and is developing bed sores, you want to question why he’s spending so much time in the same position? Even if the resident is confined to a bed, they need to be rotated every hour or two, and these rotations should be marked on the resident’s medical chart.
Are there other visitors you can talk to?
If you are able to talk to other visitors who already have a loved on there, see if you can ask them specific questions about the facility. Ask how long their family member has lived there and if they have ever noticed any red flags. Unfortunately, sometimes patients reside at a less-than-stellar facility because either they cannot afford to stay someplace better, or because a medical condition or necessary medical equipment or maintenance may require them to be there. (An example of this is that a patient with a feeding tube is required to stay at a “nursing home” and is not allowed to live in an “assisted living facility” which is typically nicer.)
Finally, you’ll want to look for safety devices as soon as you enter the facility.
Good nursing homes encourage visitors, so they need to keep their security measures as unobtrusive as possible while still maintaining a safe environment for their residents. Cameras and check-in systems can help residents stay safe without alarming or disrupting them. Light beams can monitor exits and hallways, and can even be used to alert the staff if a resident leaves his room. Many elderly folks, and particularly people in certain stages of Alzheimer’s disease are prone to wandering which can be dangerous. While the facility should not feel like a prison, the residents need to be secured for their own safety. Many facilities have secure, yet cleverly disguised, exits in their locked Alzheimer’s wings, so that the doors can’t be exited without code cards for the staff or a staff member “buzzing out” a visitor, so the wing remains secure, yet feels less like a prison.
One of the most common forms of abuse in nursing facilities is neglect. Not only nursing home neglect abusive, it’s a very serious charge. The failure of a person to receive the appropriate level of care they require considered to be neglect. Oftentimes in care facilities, neglect includes failure to assist with or provide hygiene. When residents are incapable of performing such tasks as wiping themselves after using the restroom, brushing and flossing their own teeth, bathing, washing and brushing their own hair, dressing, clipping their own fingernails and toenails, cleaning their glasses, and removing, cleaning, and reinserting their dentures, their physical health can deteriorate, and they lose their dignity which causes their self-esteem to plummet and often causes depression to set in. Furthermore, dental cavities, uncleaned private areas after restroom use, a mass of tangled or matted hair, or dirty eye glasses can cause initial discomfort to exacerbate into unbearable physical agony to these patients who may have lost the ability to communicate their agony, yet still have the ability to feel each excruciating moment.
 Too often, neglected nursing home patients are hungry and/or thirsty for hours with a tray of food sitting just out of their reach. Whether this is a deliberate “form of punishment” by a cruel staff member (such as retribution for having to clean a bathroom mess, etc.), or it’s simply an oversight by an overworked aide in an understaffed facility, the end result can be malnutrition and/or dehydration, both of which are physically painful conditions.
Too often, neglected nursing home patients are hungry and/or thirsty for hours with a tray of food sitting just out of their reach. Whether this is a deliberate “form of punishment” by a cruel staff member (such as retribution for having to clean a bathroom mess, etc.), or it’s simply an oversight by an overworked aide in an understaffed facility, the end result can be malnutrition and/or dehydration, both of which are physically painful conditions.
Some medical conditions cause elderly patients to experience difficulty swallowing. Other times, their teeth are in such a poor state that it hurts them to either bite into food or to chew the food very much. Other underlying medical conditions cause the resident to aspirate when they swallow either liquids or solids. For reasons such as these, such affected nursing home residents require more individualized attention during mealtimes. If the facility is understaffed, this can be a significant problem for these residents.
Too often, in understaffed facilities, residents don’t aren’t taken out of their bed on a daily basis, or they aren’t given the assistance they need to clean or feed themselves. Too frequently, when they are moved from their bed to a wheelchair, they are simply parked with other residents in a crowded community room with a television to “babysit” them. When this happens, the residents who are unable to utilize their muscles daily lose their mobility completely. When an elderly person fails to receive daily exercise, they lose muscle tone, strength, and balance, as well as deterioration to their circulatory system. This increases the likelihood that at some point, they will suffer from a fall, or they may develop a bedsore or other pressure infection from remaining bed-bound. Sometimes, they are medicated to keep them in bed rather than being allowed to exercise their muscles by walking or even by sitting up in a wheelchair and getting out of the four walls of their room. (Remember, even in prison, prisoners are allowed time in the yard, the cafeteria, and the commissary, and are only confined to seeing only the same four walls when they are so delinquent, they are sentenced to a period of solitary confinement.)
Unsanitary environments such as an accumulation of soiled adult diapers, bedding, or clothing, dirty floors, windows, and walls, residents who are kept in beds with sheets that are not changed regularly, or residents with clothing or adult diapers that are not changed often, and a kitchen that is not sanitized properly after each meal creates an unsafe environment for all residents. Nursing home facilities have long been known to have a prevalence of MRSA (Methicillin-Resistant Staphylococcus Aureus) infections. MRSA is a type of staph bacteria that is resistant to most of the antibiotics used to treat ordinary staph infections, and if left untreated, it often becomes fatal.
Not only can the facility’s failure to provide appropriate physical care cause the resident to suffer physical harm, but it can cause psychological damage as well. When a resident is not properly cared for, they can become fearful of the staff, feel abandoned by or resentful of the family members who committed them to the facility, and they may refuse food, hygiene, and/or other necessary care.
 Besides neglect in nursing facilities (which is also considered to be a form of abuse), other types of abuse common to nursing homes can be physical abuse, sexual abuse, and financial abuse or exploitation.
Besides neglect in nursing facilities (which is also considered to be a form of abuse), other types of abuse common to nursing homes can be physical abuse, sexual abuse, and financial abuse or exploitation.
Physical abuse of the elderly may be intentional such as a caregiver slapping, pinching, or scratching them, or (illegally) using restraints on them which can cause bruising. But it can also involve a caregiver being unaware of residents abusing each other.
Indicators* of physical abuse in a nursing facility may include:
- Traumatic hair loss
- Fractured bones
- Broken bones
- Dislocated joints
- Sprains
- Broken teeth
- Cracked teeth
- Bruises, especially hand-shaped “wrap-around” contusions or those in the shape of restraints or straps
- Welts
- Bed sores
- Unexplained loss of weight
- Changes in mental status
- Mental deterioration
- Withdrawal from visitors
*While not all patients who suffer from these signs are the victims of abuse, any of these signs should be taken as a red flag for loved ones to investigate further.
Sexual abuse of the elderly actually happens more frequently than many people realize. When an elderly resident is unable to express either consent or lack of consent, or the resident suffers from loss of cognitive skills, they make a prime target for sexual predators.
Signs of sexual abuse to the elderly can be physical as well as physiological, and may include:
- Genital bruising
- Genital or anal bleeding
- Pelvic bruising
- Pelvic fracture
- Difficulty walking
- Noticeable pain when sitting
- Diagnosis of a sexually transmitted disease
Financial abuse or exploitation of the elderly is when a caregiver or facility capitalizes on the elder’s financial accounts, or even steals from the patient, either in the form of physical theft of money or other tangible objects in the patient’s possession, or in the form of identity theft where the pirate may apply for credit using the elder’s identity.
Financial abuse or exploitation may include:
- Cashing a check made payable to the resident from their Social Security, Veterans’ Administration, Retirement Plan, Pension, or other benefits
- Cashing a resident’s check from their personal checking account
- Stealing a resident’s personal possessions
- Stealing a resident’s cash
- Forcing a resident to endorse a check made payable to the resident from their Social Security, Veterans’ Administration, Retirement Plan, Pension, or other benefits
- Forcing a resident to endorse a check from their personal checking account
- Forcing a resident to sign credit applications, bank forms, contracts, or a last will and testament
- Forging a resident’s signature on a check from their personal checking account
- Forging a resident’s signature on credit applications, bank forms, contracts, or a last will and testament
- Forging a resident’s signature on a check made payable to the resident from their Social Security, Veterans’ Administration, Retirement Plan, Pension, or other benefits
I Timothy 5:4 – “But if a widow has children or grandchildren, let them first learn to show godliness to their own household and to make some return to their parents, for this is pleasing in the sight of God.”
Call (863) 287-6388 in Polk County or (813) 287-6388 in Hillsborough County and Pinellas County today to schedule a free confidential consultation with an attorney at Your Christian Law Firm, Dean Burnetti Law.

Our Statement of Faith
We declare that Jesus Christ is the Lord of all. That the Holy Spirit abides in the midst of all within our halls. That the power of prayer is our shield and sword.
We declare that Christ is the cornerstone of this firm.
LAKELAND OFFICE:
1937 East Edgewood Drive, Suite 102,
Lakeland, Florida 33803
Lakeland: (863) 287-6388
BRANDON OFFICE:
413 Lithia Pinecrest Road,
Brandon, FL 33511
Brandon: (813) 287-6388
ST. PETE OFFICE:
11300 4th Street N., Ste. 140,
St. Petersburg, FL 33716
St. Pete: (813) 287-6388